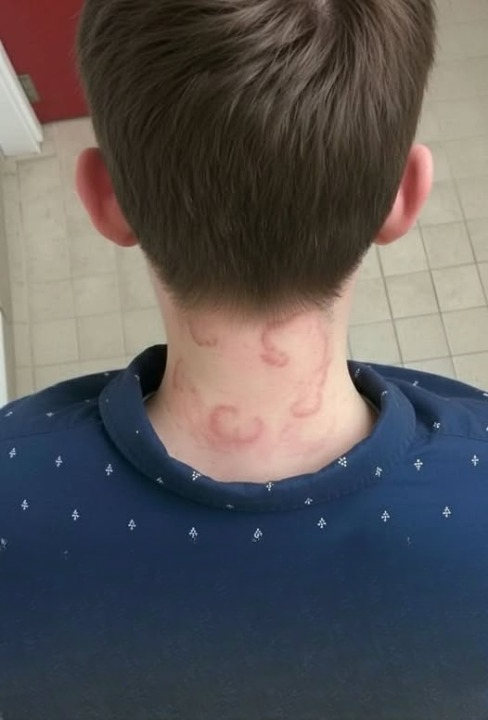
What began as a seemingly trivial itch slowly evolved into a medical concern that could no longer be ignored. Initially, it seemed harmless—a minor skin irritation that appeared sporadically, seemingly without cause.
At first, there were only small patches of redness, mild swelling, and occasional discomfort. These episodes came and went unpredictably. One moment, the skin seemed completely normal; the next, raised bumps or blotches appeared, then disappeared again as though they had never been there.
The sensations were subtle but persistent: a burning, tingling, or prickling that was irritating enough to draw attention but not yet alarming. Many parents and caregivers might dismiss such symptoms, assuming they stemmed from a temporary allergy—perhaps from a new food, an environmental exposure, or contact with an unfamiliar soap or detergent.
However, over time, it became clear that this was more than a minor, temporary reaction. What initially seemed inconsequential began developing into a recurring and increasingly widespread problem, one that required medical attention and careful management.
The Deceptive Nature of Skin Reactions
The visible skin manifestations were misleading. Small, raised patches—often pink, red, or slightly darker than surrounding skin—appeared suddenly. Some were perfectly round, others irregularly shaped, and their locations shifted from day to day.
The unpredictable pattern caused both physical discomfort and psychological stress. Not knowing when or where the next flare would occur made routine activities like playing outside, attending school, or even simple self-care increasingly stressful.
While mild, occasional skin irritation is common in children, recurring and widespread reactions like these can signal underlying immune system activity. In this case, the skin was attempting to communicate something deeper—a subtle warning from the body that it was responding inappropriately to stimuli, whether internal or external.
Diagnosis: Urticaria (Hives)
After consultation with a physician, the condition was identified as urticaria, commonly known as hives. Urticaria is not just a surface-level skin problem. It represents a complex immune-mediated reaction that primarily involves mast cells, specialized cells present in the skin and other tissues.
Mast cells play an essential role in defending the body from infections and injuries. However, in urticaria, these cells release histamine and other inflammatory mediators at inappropriate times.
When histamine enters the bloodstream, small blood vessels in the skin become leaky, allowing fluid to accumulate in the upper layers. This process creates the characteristic raised, red, itchy welts seen in hives. The reaction can range from mild and localized to severe and widespread.
When Hives Become More Serious: Angioedema
In his case, the problem extended beyond superficial hives. Swelling began to affect deeper tissue layers, including areas around the lips, eyelids, hands, and feet. This deeper swelling is medically termed angioedema.
Angioedema is particularly concerning when it involves the face, lips, tongue, or throat because it can obstruct airways and create a life-threatening emergency. Unlike the initial itch, the swelling caused sensations of tightness, puffiness, and discomfort, coupled with visible enlargement of affected areas.
The psychological impact of these symptoms was significant. What began as mild irritation had evolved into a source of fear and anxiety. Daily activities, even simple ones like speaking, eating, or swallowing, could provoke worry, as each flare carried the potential for escalation into severe allergic reactions, including anaphylaxis.
Understanding Potential Triggers
Medical professionals conducted a thorough investigation into potential triggers. Urticaria can be caused by a wide range of factors, including:
- Foods: Common triggers include nuts, shellfish, eggs, and certain additives or preservatives.
- Medications: Antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), and some pain relievers are frequent culprits.
- Infections: Viral, bacterial, or parasitic infections may provoke immune reactions.
- Physical stimuli: Pressure, heat, cold, or sunlight can lead to physical urticaria.
- Stress: Psychological stress is known to exacerbate or prolong flare-ups by affecting immune regulation.
Despite thorough evaluation, many cases remain idiopathic, meaning no definitive trigger is identified. Chronic urticaria—lasting longer than six weeks—presents additional challenges because it can persist for months or years, requiring ongoing management.
Acute urticaria, by contrast, typically resolves within six weeks and usually has identifiable triggers, making it easier to treat and monitor. Distinguishing between acute and chronic forms is crucial for planning treatment and setting expectations for families.
Treatment Approaches
Treatment focused primarily on symptom control and immune system modulation. Antihistamines are the cornerstone of therapy, often prescribed at higher doses under medical supervision for chronic or severe cases.
These medications block histamine receptors, reducing itching, redness, and swelling. In severe flare-ups, corticosteroids may be prescribed for short periods to suppress inflammation more aggressively.
Topical treatments—including soothing creams, anti-inflammatory ointments, and cooling gels—provide additional relief. However, medication alone is rarely sufficient. Education, monitoring, and lifestyle adaptations are equally important.
Vigilance and Early Recognition
Children and caregivers must learn to identify early warning signs. Even minor-looking skin reactions can signal more significant systemic involvement. This includes swelling around the face or throat, tightness in the airway, or rapid progression of hives. Prompt medical attention is critical to prevent dangerous complications.
Over time, patients develop greater body awareness, learning to recognize subtle changes that may precede a flare-up. This awareness allows for proactive management rather than reactive treatment, reducing risk and improving quality of life.
Psychological Impact
The unpredictability of hives and angioedema can create significant stress. Children may develop anxiety about eating new foods, interacting socially, or participating in routine activities, fearing a sudden flare.
Emotional resilience becomes as important as physical management. Coping strategies—support networks, stress-reduction techniques, and therapy—help mitigate anxiety, allowing children and families to maintain a sense of normalcy despite the challenges of chronic urticaria.
Lifestyle and Environmental Modifications
Lifestyle adjustments complement medical treatment and can reduce the frequency or severity of flare-ups. Strategies include:
- Dietary management: Avoiding known food triggers and maintaining a balanced, anti-inflammatory diet.
- Stress management: Mindfulness, yoga, exercise, and adequate sleep help regulate immune responses.
- Environmental protection: Loose clothing, sunscreen, and temperature regulation prevent physical triggers.
- Trigger tracking: Symptom diaries help identify patterns and guide prevention strategies.
Advanced Treatments
For cases unresponsive to standard therapies, additional options are available:
- Leukotriene receptor antagonists: Reduce immune-mediated inflammation.
- Second-generation antihistamines: Provide longer-term relief with fewer side effects.
- Biologic therapies: Omalizumab, an anti-IgE monoclonal antibody, targets specific antibodies that activate mast cells, reducing flare frequency and severity.
These treatments are typically reserved for persistent, chronic cases that fail conventional management.
Emergency Preparedness
Children at risk for severe angioedema or anaphylaxis must have an action plan:
- Epinephrine auto-injectors: Immediate intervention in emergencies.
- Education: Training in recognizing warning signs and using emergency medications.
- Communication: Teachers, caregivers, and peers should be informed to ensure prompt response during flare-ups.
Holistic Management
Effective management is multi-layered: combining pharmacological therapy, lifestyle adjustments, trigger avoidance, and psychological support.
- Regular follow-ups: Ensure medications are effective, adjust doses, and monitor complications.
- Sleep and activity regulation: Prevent fatigue and immune compromise.
- Emotional support: Counseling or support groups reduce stress and enhance coping.
- Preventive strategies: Structured routines, hydration, and awareness of environmental factors.
This comprehensive approach transforms a potentially frightening chronic condition into a manageable aspect of daily life.
Monitoring and Evaluation
Allergen testing and immunological evaluations help identify specific triggers, though idiopathic urticaria remains common. Tests include:
- Bloodwork: Identify immune abnormalities or autoimmune involvement.
- Skin prick tests: Determine reactivity to specific allergens.
- Challenge tests: Supervised exposure to suspected triggers.
These assessments allow for tailored management strategies and prevent unnecessary dietary or lifestyle restrictions.
Long-Term Outlook
Chronic urticaria and angioedema are often unpredictable but manageable. With proper care, children can lead full, active lives while minimizing risks.
Monitoring, education, and preparedness reduce the likelihood of severe flare-ups. Understanding the difference between cosmetic symptoms and dangerous reactions empowers patients and caregivers to respond appropriately.
Lessons Learned
What began as a minor, irritating itch evolved into a profound lesson in body awareness, resilience, and proactive healthcare. Chronic urticaria and angioedema highlight:
- The skin is a vital indicator of internal health.
- Early recognition and intervention can prevent complications.
- Lifestyle, medication, and emotional support must work together.
- Vigilance transforms fear into empowerment.
Ultimately, these conditions illustrate the complexity of the immune system and the importance of comprehensive, informed management.
Conclusion
Chronic urticaria and angioedema are more than skin-deep issues. They represent a delicate balance between immune response, environmental exposure, and emotional wellbeing.
Through proactive care—including medical treatment, trigger avoidance, lifestyle modifications, and psychological support—children can safely navigate the challenges of these conditions. Awareness, preparedness, and education are key to turning uncertainty into confidence, ensuring safety while maintaining quality of life.
By listening to the body, observing patterns, and responding promptly, patients and families can manage chronic urticaria effectively, transforming a frightening condition into a manageable part of daily life.
What began as a minor itch became an enduring lesson in resilience, vigilance, and the importance of understanding one’s body—a reminder that even subtle symptoms may carry significant messages about health.